International Pilonidal Sinus Disease Conference
23 September 2017 BERLIN
International Pilonidal Sinus Disease Conference
Hotel Grunewald, Kronprinzessinnenweg 120, Berlin, Germany
The room was full with almost 100 attendees. Registrations closed 2 weeks before the conference. Several speakers enjoyed a wonderful pre-conference dinner sponsored by ACELITY at Haus Sanssouci.

Session 1 started only 5 minutes late despite some fairly significant technical difficulties – nothing that a taxi and a laptop running Windows 98 could not overcome!

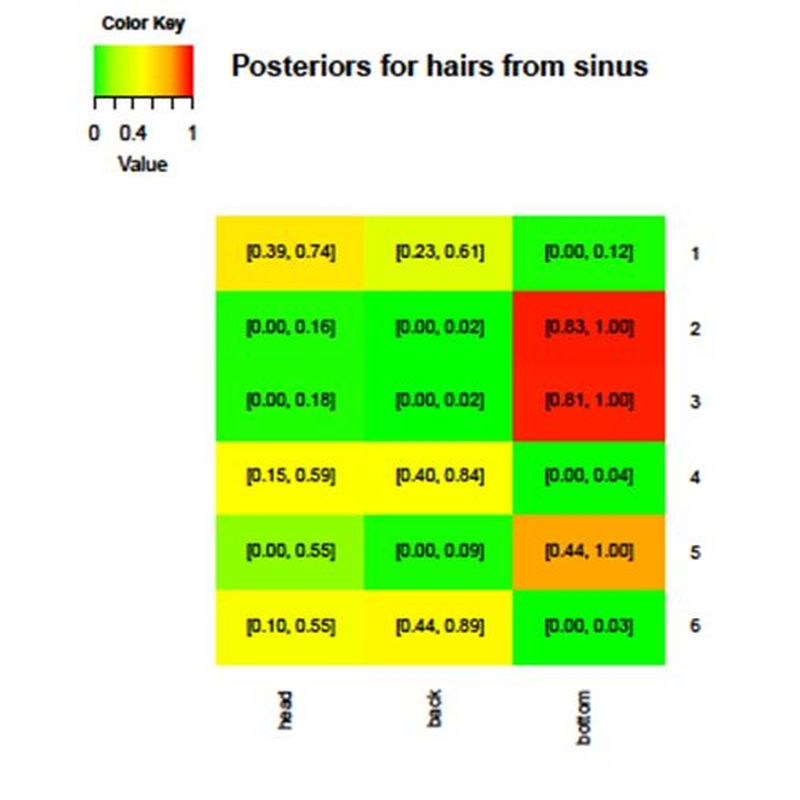
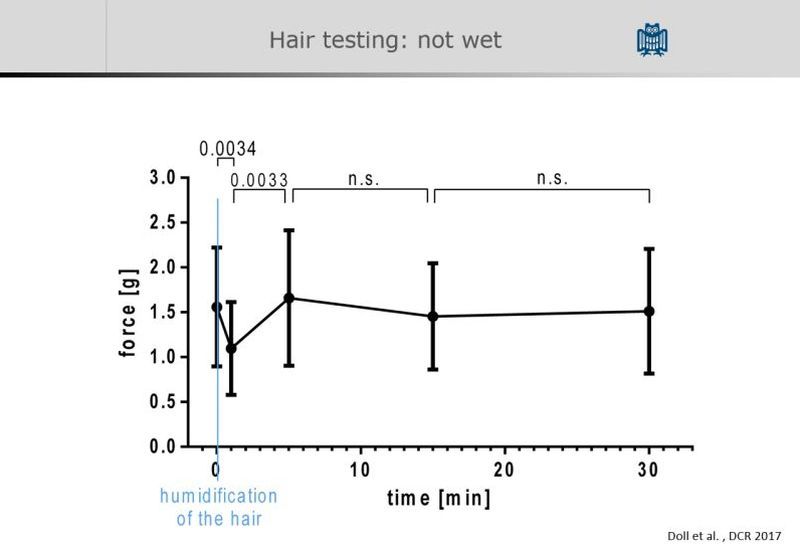
Friederike Bosche performed force value experiments. She showed heatmap diagrams demonstrating pilonidal disease hairs are not from the intergluteal fold but occipital in origin. Vast majority of hairs were rootless and shorter than 1 cm in length.
Burhan Kanat illustrated the long history of pilonidal disease starting in 1833 with Herbert Mayo.

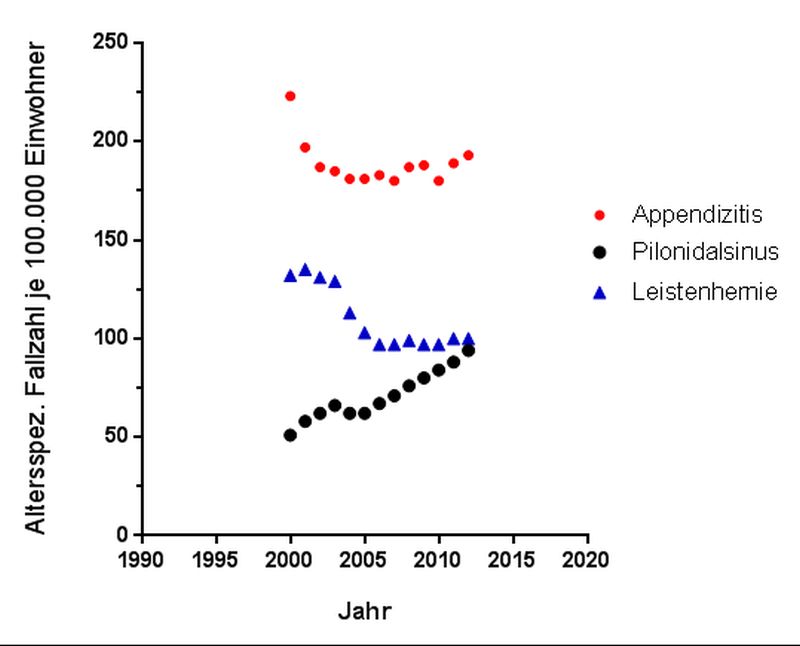
Dietrich Doll showed several graphs: incidence of PSD is increasing especially in those aged 20 to 30 years.
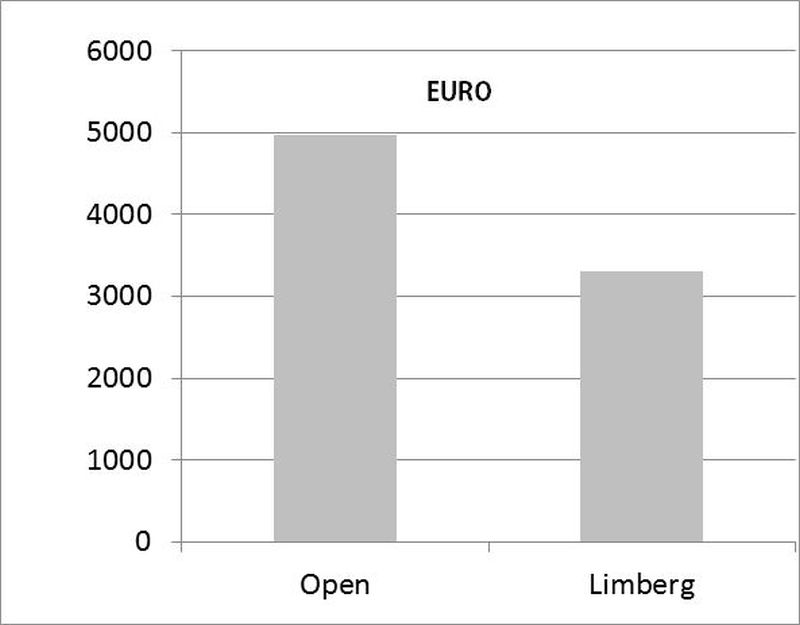
Sven Petersen showed costs are lower with flaps compared to open healing. This relates to open healing often taking 2 to 3 months.
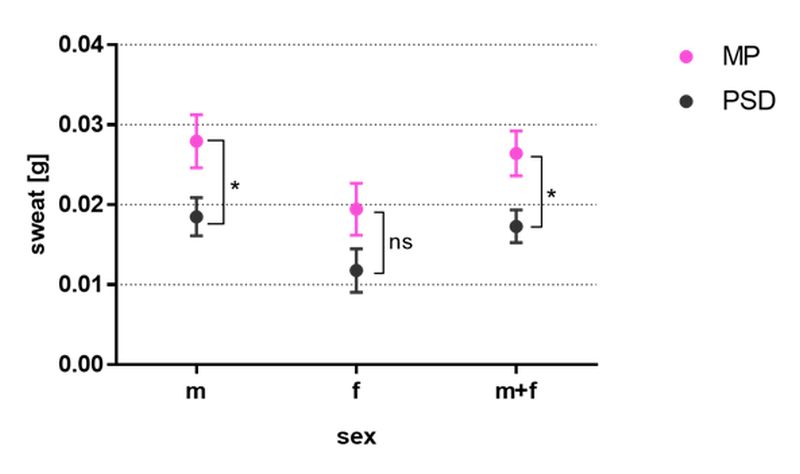
Dietrich Doll confirmed males sweat more than females but surprised the audience by stating PSD patients sweat less than matched controls!
Diego Segre compared PSD patients with Hidradenitis suppurativa – the key differential.

Dietrich Doll illustrated the trends in recurrence – the longer the follow up the greater the pick up rate.
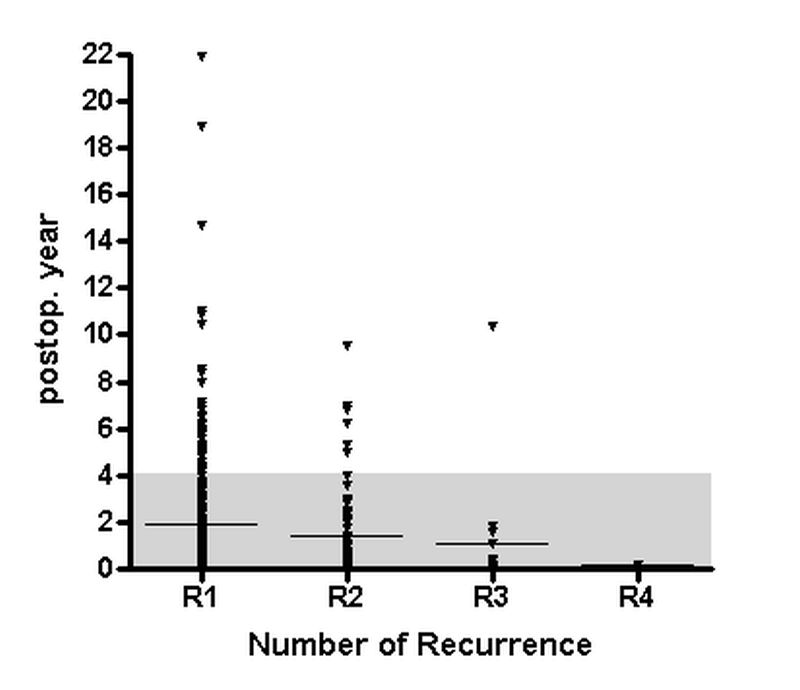
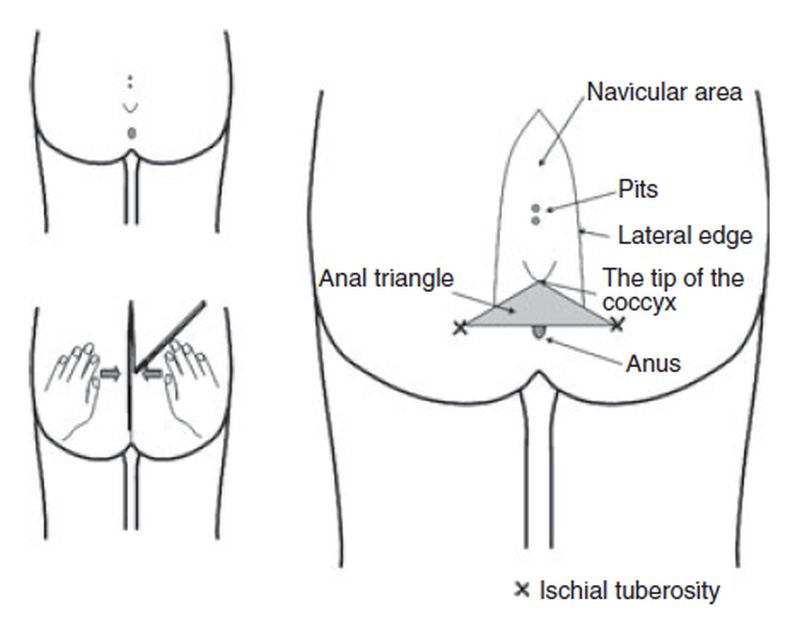
There were two presentations on Pilonidal Disease classification. Ekmel Tezel (navicular concept) and Ali Guner's talks were followed by lively discussion. A live survey followed. Many suggested an internationally recognized classification is necessary.

We rounded off the morning session with Guidelines from Germany and Italy by Igors Iesalnieks and Luigi Basso. We have more in common than we suspected!

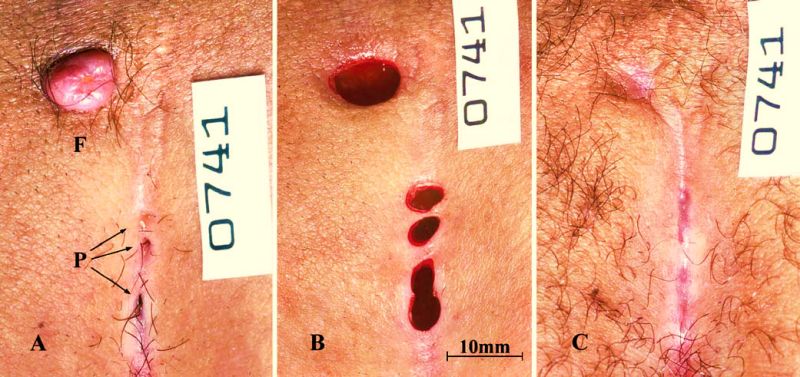
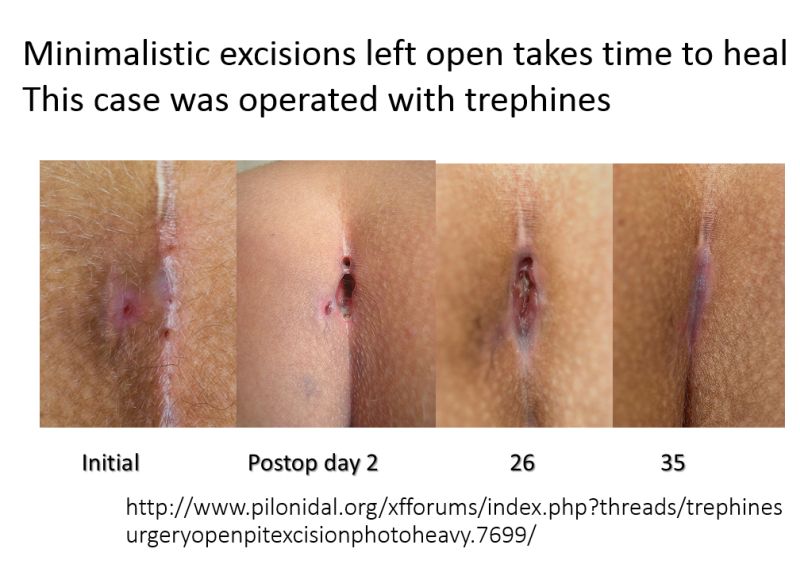
After morning tea, it was the How I Do It session. Moshe Gips presented 13.2% recurrence rate at 5 years (and 16.2% at 10 years) using minimal excision with trephines.
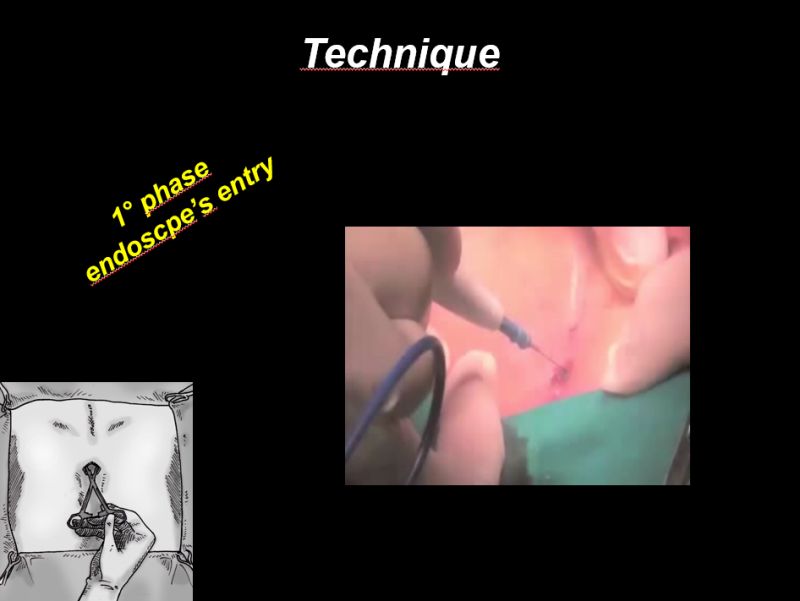
Marco Milone showed patients managed with EPSiT experienced less pain and greater satisfaction than management with cleft lift.
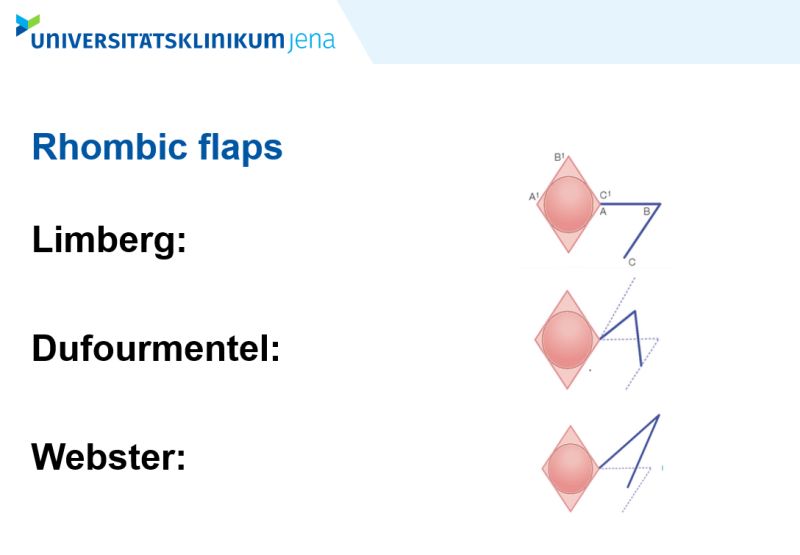
Michael Ardelt presented a rhombic flap overview as well as his Limberg Flap results.
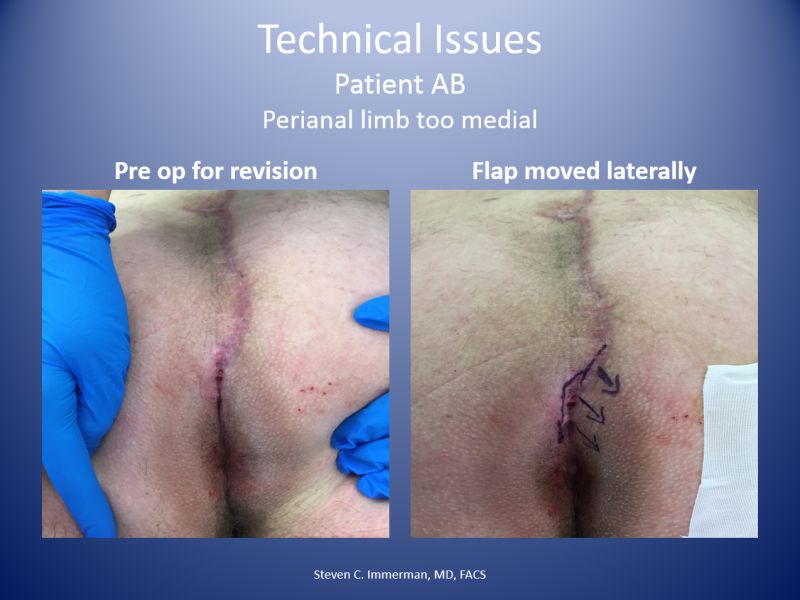
Steven Immerman showed how he manages patients with perianal PSD: 110 patients with 98% recurrence free at long term follow-up using Bascom cleft lift. Some patients required revision of the lower scar due to it being too medial.
Asha Senapati also presented great results following Bascom cleft lift in patients with recurrent disease.
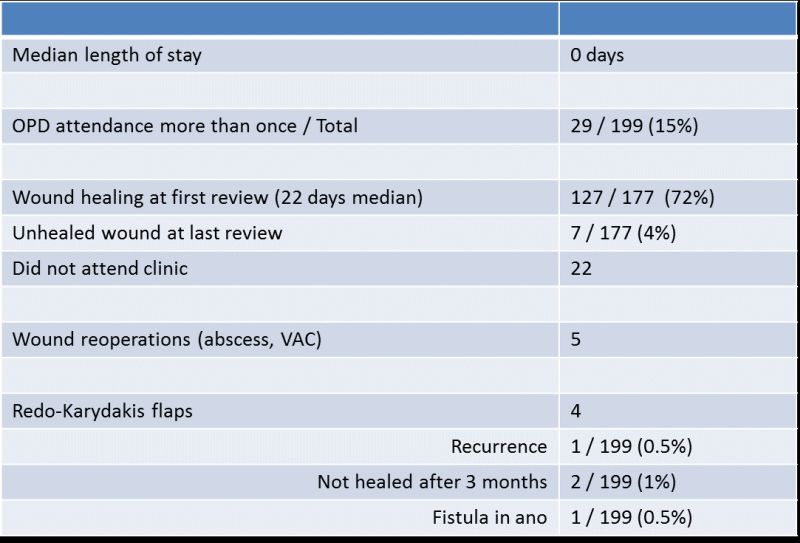
Peter Wysocki showed Karydakis flap learning curve is between 10 and 20 operations. At long term follow-up in 199 patients recurrence was observed in 0.5%.
Jonas Kolbenschlag presented larger and unconventional flaps that plastic surgeons at times undertake.
Roland E Andersson showed 27% recurrence rate after 3.3 years with the modified Lord–Millar technique (i.e. closure of midline excisions but leaving the cleansed lateral opening open).
The session was rounded off by Markus Lüdi who told us about anaesthetic issues.

After lunch, Peter Kauf presented Statistics and showed the usefulness of heatmaps when presenting data graphically.
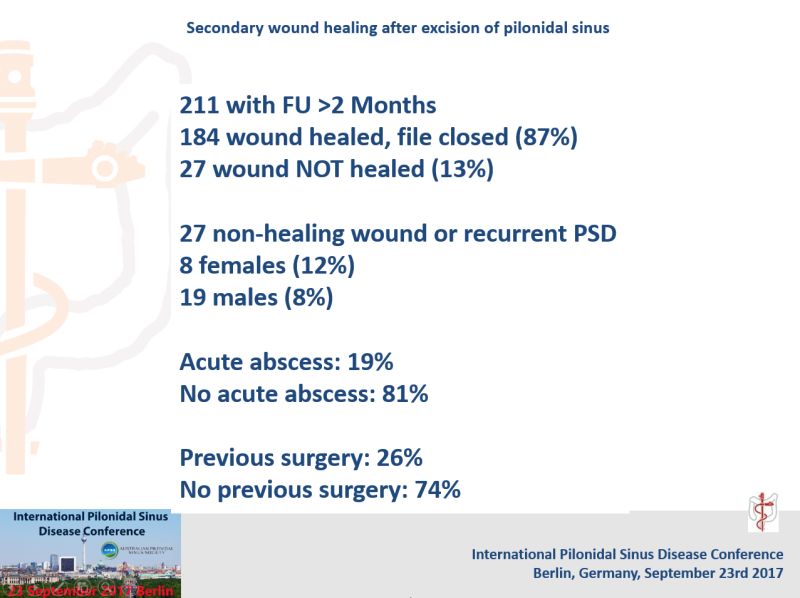
Johannes Jongen showed that 13% of wounds had not healed by 2 months after primary open treatment.
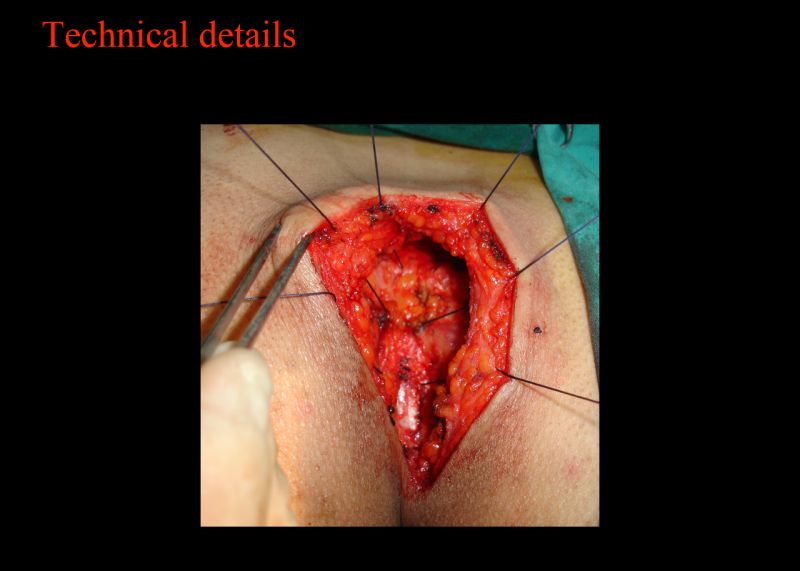
Fatih Altintoprak showed Tension-free primary midline closure.
Igors Iesalnieks showed recurrence after Pit picking increases with length of followup.
Cüneyt Kayaalp showed 70% success rate with first round of liquid phenol.
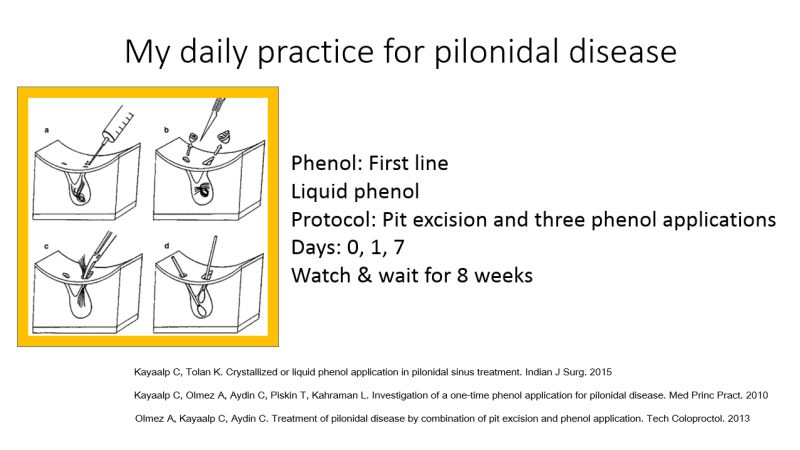
Mustafa Girgin demonstrated great results with crystallized phenol but seems this form of pehol is not widely available. Hairy males responded to treatment better than glabrous females.

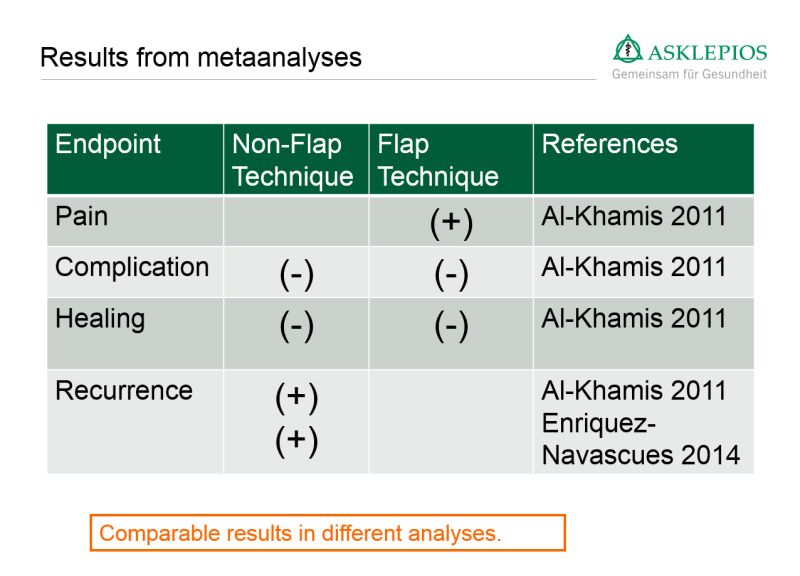
Sven Petersen showed that outcomes for flap repair are better than for vs non-flap techniques.
Ekmel Tezel'sTreatment algorithm is based on his classification system. Cleft Lift is frequently used.
Moshe Gips advises his patients to postoperatively avoid Sitz baths but instead flush their wounds with running water several times each day. Patients usually resume regular activity within three days of punch excisions. For open wounds, a dressing which keeps buttocks apart is needed.
Vahit Onur Gul showed the commonest site of extrasacrococcygeal PSD is umbilicus – this is often managed with local wound care.
Shirley Chan and David Armstrong showed how nonhealing pilonidal wounds respond to 10% metronidazole ointment (Ortem).
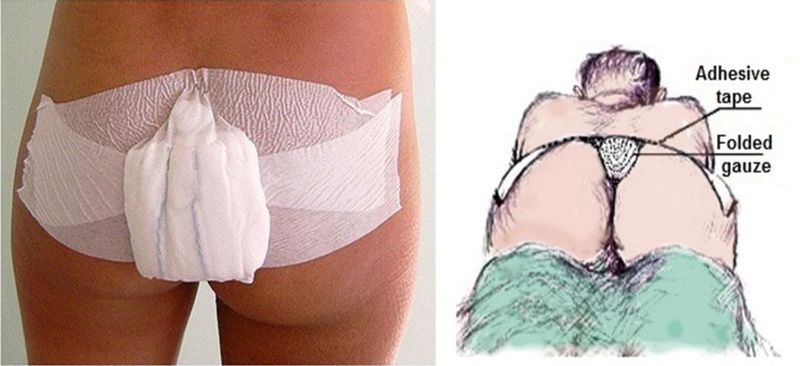
After afternoon tea, Dietrich Doll demonstrated that while society’s BMI is steadily increasing, the incidence of PSD is males is increasing at a quicker rate. Incidence of PSD is increasing in all age groups except for those over 65 years.
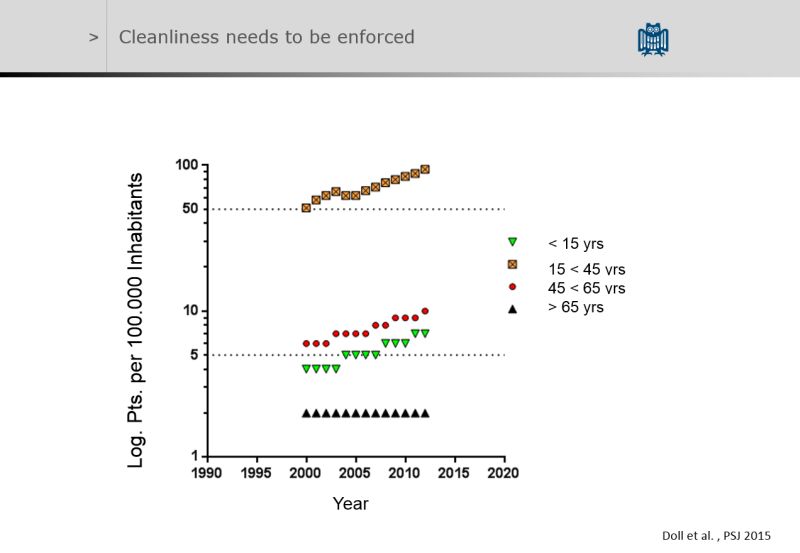
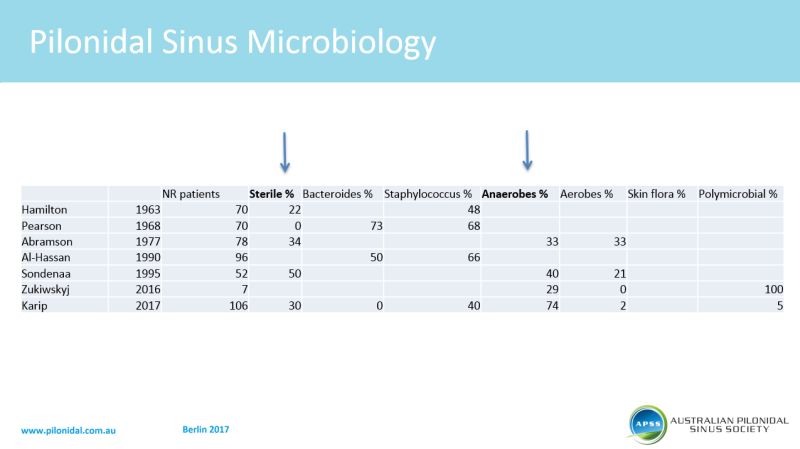
Peter Wysocki shoved that less than 20% of patients after pilonidal abscess drainage required further surgery at 7 years followup. Healing was quicker in off-midline drainages. Pilonidal wounds often contain gram negatives, anaerobes and Staphylococci. One third of wounds show no bacterial growth.
Verena Stauffer not only showed that recurrence rate relates to choice of treatment and follow-up but finished the scientific session with a wonderful summary of outcomes.
Dietrich Doll summarised that best long term results are obtained with asymmetric techniques: Karydakis/Bascom, Limberg/Dufourmentel and other flaps (these have a 1% per year recurrence rate).
There were many free paper presentations: Indian Seton, Modified EPSiT, ultrasonic curettage, 15 Years Karydakis flap follow-up, endoscopic abscess drainage, Dermatotraction, 192 Limberg flaps for recurrent PSD, PSD fistula in ano, Intermammary PSD and finally Friederike Bosche presented on hair strength.
We ended this massive day with photos outside and discussions about the future: classification, studies, international society and meeting again.

Look forward to meeting all of you again in a few years’ time!

